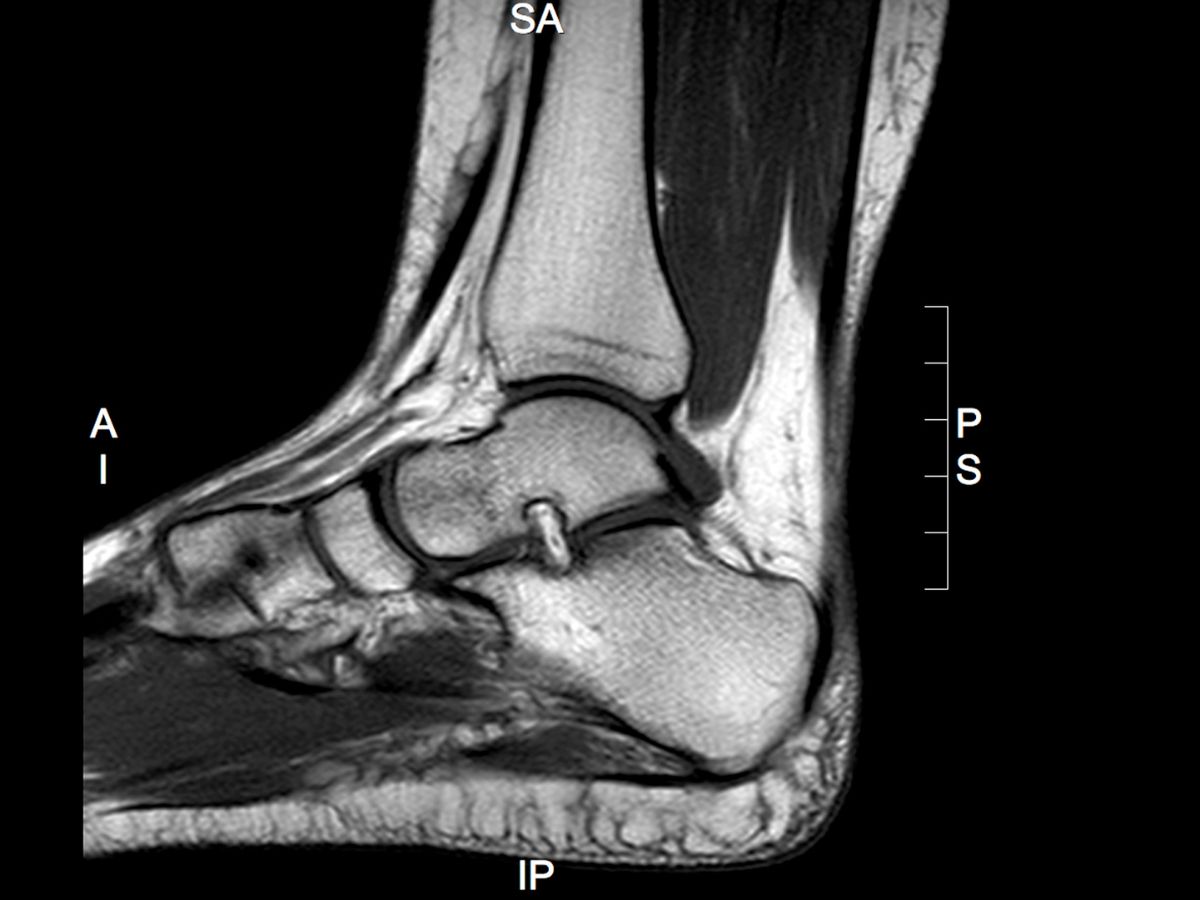
Magnetic resonance imaging (MRI) plays an important role in the assessment of foot and ankle conditions, particularly where more detailed evaluation of soft tissue and intra-articular structures is required. While not all patients need advanced imaging, understanding when to refer for MRI is key to improving diagnostic accuracy and guiding appropriate management.
MRI provides detailed visualisation of both soft tissue and bone, making it particularly useful in complex or persistent presentations. It is commonly indicated in cases of ongoing pain where initial management has failed, or where clinical examination and first-line imaging do not fully explain the patient’s symptoms. This includes suspected tendon pathology, ligament injury, osteochondral lesions, stress reactions or fractures, and joint pathology.
In the context of ankle injuries, MRI can be valuable in identifying associated injuries that may not be evident on initial assessment, such as osteochondral defects, syndesmotic injury, or tendon pathology. In forefoot and midfoot conditions, it can help differentiate between soft tissue, bony, and joint-related causes of pain, particularly where symptoms are not following an expected clinical course.
MRI is also useful in evaluating inflammatory and systemic conditions affecting the foot and ankle. It can detect early changes in inflammatory arthropathies, bone marrow oedema, and other features that may not be visible on radiographs. In patients with atypical presentations or suspected systemic disease, MRI can therefore provide important diagnostic information.
Referral for MRI should be considered where there is diagnostic uncertainty, failure of appropriate conservative management, or where imaging findings will influence clinical decision-making. It is particularly valuable when planning further interventions, including injection therapies or surgical management, where a clear understanding of underlying pathology is required.
It is important to recognise that MRI should not be used in isolation. Findings must be interpreted in the context of the clinical picture, as incidental abnormalities are common and may not be the primary source of symptoms. A structured approach to assessment remains essential to avoid over-investigation and unnecessary intervention.
Multidisciplinary team (MDT) working enhances the value of MRI in clinical practice. Collaboration between radiology, podiatry, physiotherapy, orthotics, and orthopaedic surgery allows imaging findings to be integrated into a comprehensive management plan, particularly in complex or persistent cases.
For clinicians, understanding when MRI is indicated helps ensure appropriate use of advanced imaging and supports more confident decision-making. For patients, timely referral for MRI can lead to more accurate diagnosis, targeted treatment, and a more structured approach to care when initial management has not been successful.